How Thermal and Mechanical Forces Impact Zygomatic Implant Success
Key Factors Behind Successful Zygomatic Implants

Zygomatic implants have transformed the management of patients with severe maxillary bone loss, offering a reliable alternative where conventional implants are not viable. Anchored in the dense zygomatic bone, these implants provide enhanced stability and allow for full-arch rehabilitation without extensive grafting procedures. However, their success depends on more than surgical skill alone.Among the many variables influencing outcomes, thermal and mechanical forces play a decisive role during placement, healing, and long-term function. Excessive heat generation or poorly managed mechanical stress can compromise osseointegration, reduce implant stability, and increase the risk of complications. Understanding how these forces interact with bone biology is essential for clinicians aiming to achieve predictable, long-lasting results with zygomatic implants.
Understanding Zygomatic Implants: A Clinical Overview
Zygomatic implants are extra-long implants designed to engage the zygomatic bone rather than relying solely on the maxillary alveolar ridge. This approach is particularly beneficial for patients with advanced bone resorption, sinus pneumatization, or previous graft failures.
Key Clinical Characteristics Include:
- Implant lengths typically ranging from 30 to 52.5 mm
- Engagement with high-density cortical bone
- Angulated placement traversing the maxillary sinus or sinus wall
Unlike conventional implants, zygomatic implants are exposed to higher biomechanical demands due to their length and angulation. Centres offering advanced treatments such as dental implant Leeds services often emphasise meticulous planning to address these challenges. The interplay between surgical technique, bone response, and prosthetic loading is especially critical in ensuring long-term success.
Thermal Forces in Zygomatic Implant Placement
1. Sources of Thermal Stress
Thermal stress is primarily generated during osteotomy preparation. The dense nature of the zygomatic bone increases friction during drilling, which can elevate temperatures if not properly controlled.
Common Contributors Include:
- High drill speeds combined with excessive pressure
- Prolonged drilling time
- Dull or worn surgical burs
- Inadequate irrigation
Given the length of osteotomies required for zygomatic implants, cumulative heat generation becomes a significant concern.
2. Biological Impact of Excessive Heat
Bone tissue is highly sensitive to temperature increases. Research indicates that temperatures exceeding 47°C for even short durations can result in irreversible bone damage.
Potential Consequences Include:
- Bone necrosis at the implant interface
- Impaired osseointegration
- Delayed or failed healing
- Increased susceptibility to infection
For clinics providing Zygomatic Dental Implants Leeds, strict adherence to thermal control protocols is essential to preserve bone vitality and promote successful integration.
3. Strategies to Minimise Thermal Damage
Effective thermal management relies on a combination of technique and technology:
- Copious external and internal saline irrigation
- Intermittent drilling to allow heat dissipation
- Use of sharp, well-maintained drills
- Optimised drilling sequences and reduced rotational speed
These measures significantly reduce thermal trauma and enhance biological outcomes.
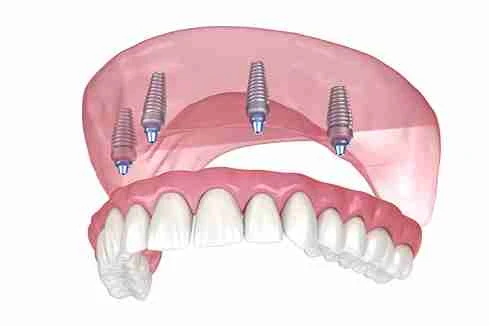
Mechanical Forces Affecting Zygomatic Implants
1. Primary Stability and Load Distribution
Primary stability is a cornerstone of zygomatic implant success. The dense cortical structure of the zygomatic bone offers excellent anchorage, but implant design and placement angle heavily influence load distribution.
Factors Affecting Stability Include:
- Bone density and quality
- Implant length and diameter
- Insertion torque values
- Bicortical engagement
When properly planned, zygomatic implants can achieve high primary stability, even in complex anatomical scenarios.
2. Occlusal Forces and Functional Loading
Once restored, zygomatic implants are subjected to substantial occlusal forces. These forces are often greater than those experienced by conventional implants due to cantilever effects and angulated prosthetic designs.
Key Considerations Include:
- Direction of masticatory forces
- Parafunctional habits such as bruxism
- Immediate versus delayed loading protocols
Centres specialising in advanced rehabilitation, including Dental Implant Leeds practices, often favour splinted prosthetic designs to distribute forces evenly across the implant framework.
3. Micromovement and Implant Failure
Excessive micromovement during the healing phase can prevent stable osseointegration, leading to fibrous tissue formation around the implant.
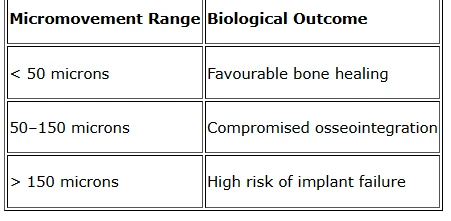
Controlling mechanical stress during early healing is therefore critical for long-term implant survival.
Interaction Between Thermal and Mechanical Factors
Thermal and mechanical forces are not isolated variables; they often influence one another. Thermal damage can weaken bone structure, reducing its ability to withstand mechanical loads. This compromised bone may fail to provide adequate primary stability, increasing the risk of micromovement.Conversely, excessive insertion torque applied to compensate for poor stability can further stress thermally injured bone. In treatments involving zygomatic dental implants Leeds, clinicians must recognise this interaction and adopt a balanced approach that prioritises both biological preservation and mechanical optimisation.
Surgical and Prosthetic Considerations to Optimise Success
Successful zygomatic implant therapy depends on precise planning and execution across both surgical and prosthetic phases.
Key Optimisation Strategies Include:
- Preoperative CBCT analysis for accurate anatomical mapping
- Digital planning and guided surgery to control angulation
- Avoidance of excessive cantilevers in prosthetic design
- Rigid, splinted frameworks to distribute occlusal forces
Prosthetic materials and occlusal schemes should be carefully selected to minimise stress concentration, particularly in patients with high bite forces or parafunctional habits.
Clinical Implications and Future Perspectives
Zygomatic implantology is advancing rapidly, with emerging technologies helping clinicians better manage thermal and mechanical challenges during treatment. These innovations are improving surgical accuracy, reducing biological risks, and enhancing long-term implant success. Continued research is also shaping safer, more predictable clinical protocols for complex cases.
Key Advancements Include:
- Dynamic navigation systems for precise implant placement
- Enhanced implant surface treatments to support osseointegration
- Real-time torque monitoring to control mechanical stress
- Ongoing studies on bone biomechanics and thermal thresholds
Together, these developments are reducing complications, improving outcomes, and expanding treatment accessibility.
Conclusion
Thermal and mechanical forces play a pivotal role in determining the success of zygomatic implants. Excessive heat during osteotomy preparation can compromise bone vitality, while unmanaged mechanical stress can disrupt osseointegration and long-term stability. By understanding the interaction between these forces and applying meticulous surgical and prosthetic strategies, clinicians can significantly improve patient outcomes. At Smilo Dental Implant Leeds, a commitment to evidence-based protocols and advanced planning ensures that zygomatic implant treatments are delivered with precision, safety, and long-term success at the forefront.
0 comments
Log in to leave a comment.
Be the first to comment.