Glass Prescription vs. Eye Disease Diagnosis: Who Handles What?
Glass Prescription vs. Eye Disease Diagnosis: Who Handles What?

You went in for blurry vision and left with a glasses prescription. But did your eye doctor check for glaucoma, examine your optic nerve, or look for early signs of diabetic eye disease? Most people don’t realize that the type of eye doctor they see determines far more than just their prescription.
This confusion is common. In the U.S., there are three types of eye care professionals, optometrists, ophthalmologists, and opticians and each plays a very different role. Mixing them up isn’t just confusing, it can impact your vision.
This guide explains who prescribes glasses, who diagnoses eye diseases, what each exam includes, and when to move from a routine check to a specialist.
The Three People in Your Eye Care Team (and What Each One Actually Does)
Most people think of “the eye doctor” as a single role. In reality, there are three distinct professionals, each with a defined scope of practice set by state licensing boards. Understanding this matters, because going to the wrong one for your specific concern can delay a diagnosis that could protect your sight.
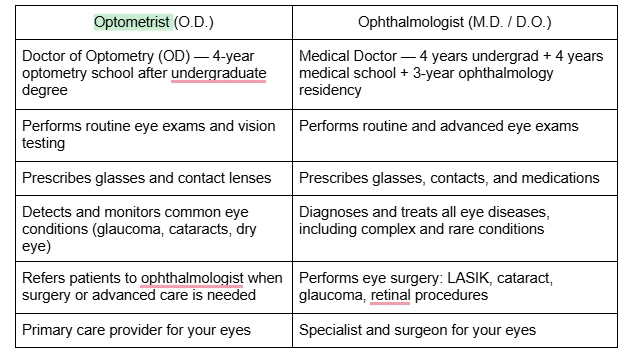
Opticians are different from both. They are trained to fit and dispense eyeglasses and contact lenses based on prescriptions written by optometrists or ophthalmologists. They cannot examine your eyes, diagnose any condition, or write prescriptions.
Who Prescribes Your Glasses? The Role of an Optometrist in Vision Correction
When your vision is blurry and you need new lenses, your optometrist is typically your first stop and in most cases, the right one. Here is exactly what a standard glasses prescription eye exam involves, so you know what you are paying for and what to ask about.
What Is Included in a Glasses Prescription Eye Exam?
A comprehensive eye exam at an optometrist’s office is not just about reading letters off a chart. A thorough exam includes:
- Visual acuity testing — measures how clearly you see at various distances using the standard letter chart (Snellen chart) and near vision chart.
- Refraction assessment — determines your exact prescription using a phoropter, the device with rotating lenses where your doctor asks “Which is better, 1 or 2?” This identifies your degree of nearsightedness (myopia), farsightedness (hyperopia), and astigmatism.
- Cover test and eye alignment check — evaluates how well your eyes work together to detect conditions like strabismus (crossed eyes).
- Slit-lamp examination — uses a high-powered microscope to examine the front of your eye, including the cornea, iris, and lens, to detect early cataracts, corneal abrasions, or inflammation.
- Intraocular pressure (IOP) measurement — the “puff of air” test or a contact tonometer checks the fluid pressure inside your eye. Elevated IOP is a major risk factor for glaucoma.
- Dilated fundus exam (if performed) — pupils are dilated with eye drops to give the doctor a wider view of the retina, macula, and optic nerve. This is where signs of retinal damage, macular degeneration, or early glaucoma can be spotted.
At the end of a refraction exam, your doctor writes a prescription that includes numbers for sphere (SPH), cylinder (CYL), axis, and sometimes an add power for bifocals. You can then take this prescription to any optician or eyeglass retailer to have your lenses made. The prescription is yours by law.
Eye Disease Diagnosis: What Your Optometrist Can Catch
Here is where things get more nuanced and where getting the right care really matters. Both optometrists and ophthalmologists can identify signs of eye disease. But their capacity to confirm, treat, and manage those diseases is very different.
What Can an Optometrist Diagnose?
During a comprehensive exam, optometrists are trained to detect and monitor a wide range of conditions:
- Glaucoma suspects — elevated IOP, suspicious optic nerve appearance, or abnormal visual fields that require monitoring
- Early cataracts — lens clouding visible under a slit lamp
- Dry eye disease — tear film evaluation and symptom assessment
- Diabetic retinopathy — signs of blood vessel damage in patients with diabetes
- Age-related macular degeneration (AMD) — drusen deposits and pigment changes in the macula
- Hypertensive retinopathy — changes to retinal blood vessels in patients with high blood pressure
- Conjunctivitis, styes, and other external eye infections
Can an Optometrist Diagnose Glaucoma?
This is one of the most searched questions in eye care and the answer is: yes, in many cases. Optometrists are trained to perform the standard diagnostic tests for glaucoma, including:
- Tonometry — measures intraocular pressure (normal range: 10–21 mmHg; elevated IOP raises suspicion for glaucoma)
- Ophthalmoscopy — examines the optic nerve head for cupping (the cup-to-disc ratio; a ratio above 0.6 is often considered suspicious)
- Visual field testing (perimetry) — maps peripheral vision loss, the hallmark functional deficit of glaucoma
- Optical coherence tomography (OCT) — an advanced imaging scan that measures the thickness of the nerve fiber layer around the optic disc, which thins progressively with glaucoma damage.
Optometrist vs. Ophthalmologist for Eye Exam: When Do You Need Which?
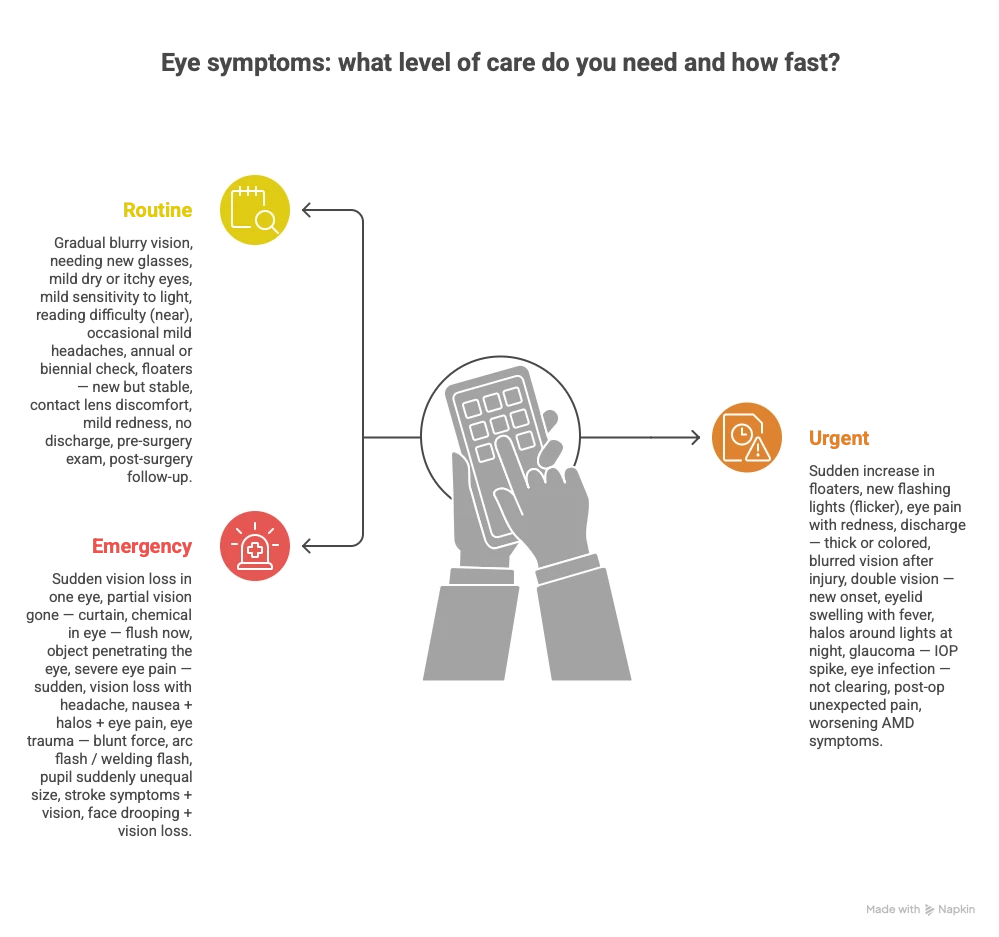
Think of it this way: your optometrist is like your primary care physician for your eyes. Your ophthalmologist is the specialist you get referred to when something beyond routine care is needed. Most people do not need to see an ophthalmologist annually. But some people absolutely should.
See an Optometrist When:
- You need a routine annual or biennial eye exam
- Your glasses or contact lens prescription needs updating
- You have mild dry eye, eye redness, or irritation
- You want a baseline screening for glaucoma or other diseases
- You need pre-op or post-op monitoring for eye surgery done by an ophthalmologist
- You have a family history of eye disease and want regular monitoring
See an Ophthalmologist When:
- You have been diagnosed with or are suspected of having glaucoma that requires treatment beyond monitoring
- You need cataract surgery evaluation or surgery
- You are considering LASIK or other refractive surgery
- You have been diagnosed with diabetic retinopathy and need laser treatment or injections
- You experience sudden vision changes, flashes of light, or floaters (possible retinal detachment)
- You have an eye injury or chemical exposure requiring surgical or advanced medical care
- Your optometrist refers you for a second opinion or specialized treatment
What Does Your Glasses Prescription Actually Mean?
A lot of people pick up their glasses prescription and have no idea what the numbers mean. Here is a straightforward breakdown so you can actually understand your own eye health data.

How Eye Disease Changes What Your Exam Includes
If you have a known risk factor or a pre-existing eye condition, your exam is not the same as a routine vision check. Your doctor will add specific diagnostic tests based on your clinical picture. Here is what changes when disease is in the picture:
For Diabetic Patients
Diabetic eye exams require dilation every visit to evaluate the retina for microaneurysms, hemorrhages, or neovascularization. If advanced diabetic retinopathy is detected, fluorescein angiography, a procedure that uses an injectable dye to map retinal blood vessels, may be ordered. Treatment with anti-VEGF injections (such as Avastin or Eylea) is performed by a retinal ophthalmologist, not an optometrist.
For Glaucoma Suspects or Diagnosed Patients
Your exam will include not just IOP measurement and fundus photography, but a 24-2 or 10-2 visual field test, OCT of the retinal nerve fiber layer (RNFL), and Heidelberg retina tomograph (HRT) imaging of the optic nerve head in more advanced monitoring centers. These tests are compared over time to track disease progression.
For Cataract Patients
When cataracts are significant enough to impair daily function, you will be referred to an ophthalmologist for a surgical evaluation. This includes corneal topography, axial length measurement with optical biometry (used to calculate intraocular lens power), and specular microscopy to assess corneal endothelial cell health before surgery.
Conclusion
The difference between a glasses prescription and an eye disease diagnosis is not just technical — it is the difference between clear vision today and protected vision for life. Knowing who to see, what tests to ask for, and when a referral is warranted puts you in control of your own eye health journey.
Southwest Florida Eye Care (SW FL Eye Care) is proud to offer its services across Fort Myers, Cape Coral, and Naples, FL, with a team of both experienced optometrists and board-certified ophthalmologists who work together in exactly the co-management model described in this guide.
If you are unsure whether you need an optometrist or an ophthalmologist or if it has been more than a year since your last comprehensive eye exam, do not wait for symptoms to appear. Most serious eye diseases give no warning until damage is done. We have a team of ophthalmologists and optometrists in Naples, so no matter what you need, you are in the right place.
Call us today to schedule your comprehensive eye exam at our eye care in Naples.
Frequently Asked Questions
1. How Often Should Adults Over 60 Get a Comprehensive Eye Exam?
Adults 65+ should get an eye exam every 1–2 years, even without symptoms. Those with diabetes, high blood pressure, or a family history of eye disease should go annually.
2. Does Insurance Cover Eye Exams Differently for Glasses vs. Medical Issues?
Yes. Vision insurance covers glasses prescriptions (refraction), while medical insurance covers exams for conditions like glaucoma or diabetic eye disease. Some patients may use both in one visit.
3. What Is the Difference Between Intraocular Pressure and Eye Strain?
IOP is pressure inside the eye; high levels can damage the optic nerve. Eye strain is muscle fatigue from screen use. Sudden high IOP can cause pain and headaches, while chronic high IOP often has no symptoms.
4. Can Children See an Optometrist or Need a Pediatric Ophthalmologist?
Most children can see an optometrist for routine care. More serious conditions (like strabismus or cataracts) require a pediatric ophthalmologist. First exams are recommended at 6 months, 3 years, and before school.
5. What Is OCT and When Is It Needed?
OCT (Optical Coherence Tomography) is a scan that shows detailed images of the retina and optic nerve. It’s used to detect conditions like glaucoma or macular degeneration and is usually covered when medically necessary.
0 comments
Log in to leave a comment.
Be the first to comment.