What Are ABA Therapy Billing Services?
ABA Therapy Billing Services
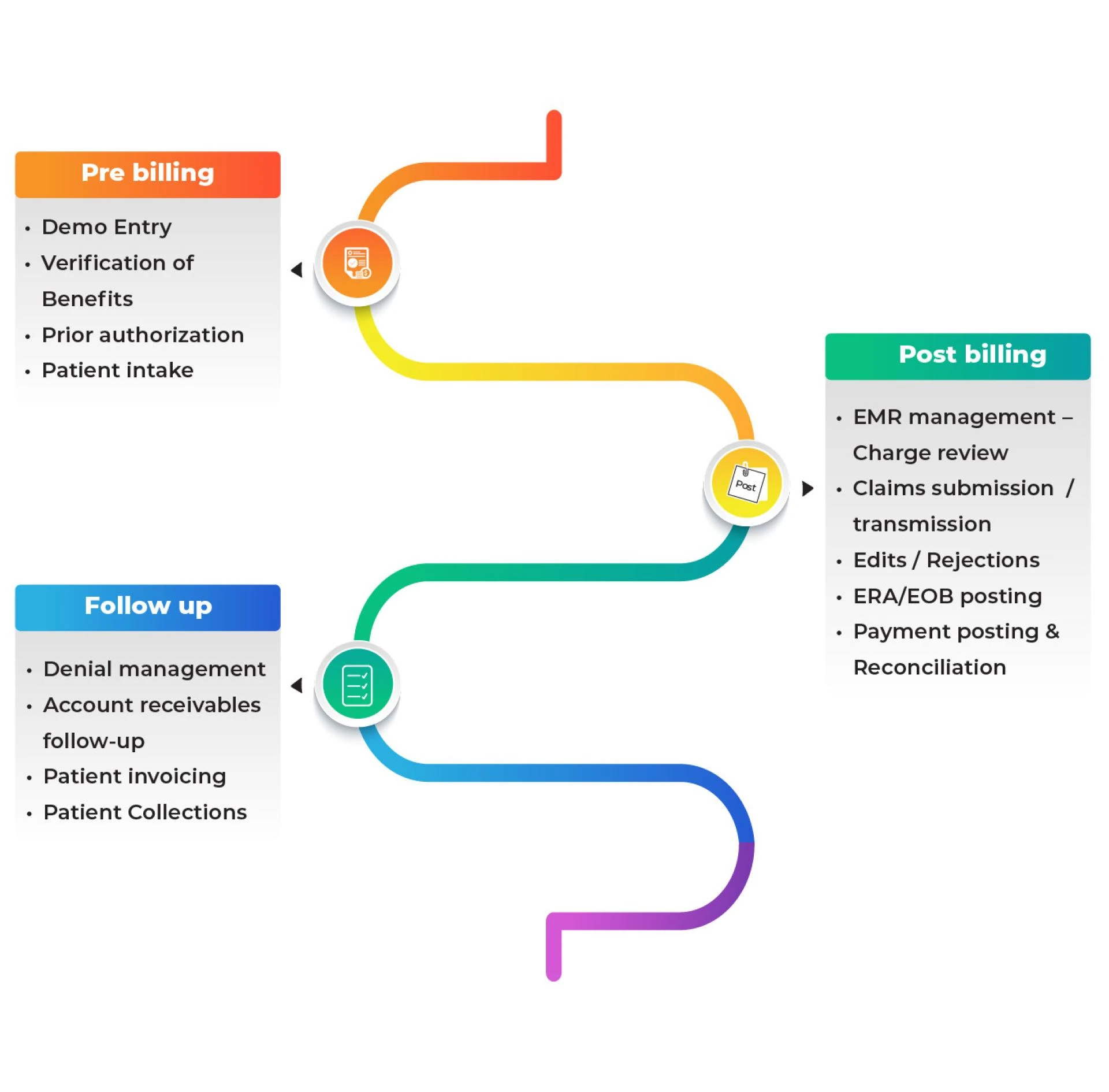
ABA therapy billing services refer to specialized medical billing processes tailored for ABA therapy practices. Unlike general medical billing, ABA billing comes with unique codes, compliance requirements, and payer-specific rules. A billing service provider ensures that all claims are accurately submitted, tracked, and reimbursed in a timely manner.
These services usually include:
- Verification of Benefits (VOB): Confirming patient eligibility and insurance coverage before therapy begins.
- Pre-Authorization Management: Securing prior authorization from insurance companies for treatment plans.
- Accurate Coding: Using proper CPT and HCPCS codes for ABA therapy sessions to avoid denials.
- Claims Submission & Follow-up: Submitting clean claims electronically and tracking them until payment is received.
- Denial Management: Identifying, correcting, and resubmitting denied claims.
- Payment Posting: Recording payments from insurance and patients for accurate financial tracking.
- Compliance Management: Ensuring adherence to HIPAA and payer-specific regulations.
WhyABA Therapy BillingIs Challenging
Billing for ABA services is more complicated than most other medical specialties due to several factors:
- Frequent Policy Updates: Insurance payers often change rules around ABA coverage, including eligibility, session length, and service limits.
- Complex Coding: ABA therapy uses specific CPT codes (like 97151, 97153, 97155, 97156) that must be applied correctly depending on the type of service.
- Prior Authorizations: Most insurers require pre-authorization for ABA sessions, and missing documentation can result in claim denials.
- High Denial Rates: Incorrect coding, missing documentation, or exceeding authorized session limits can lead to frequent claim rejections.
- Time-Intensive Process: Managing billing in-house requires extensive administrative work, pulling providers away from patient care.
Because of these challenges, many ABA providers either hire dedicated billing teams or outsource to professional ABA billing service companies.
Key Components of ABA Therapy Billing Services
1. Verification of Benefits (VOB)
Before beginning therapy, it is essential to confirm the patient’s insurance coverage. VOB involves checking:
- Whether ABA therapy is covered under the plan.
- The number of authorized hours.
- Copays, deductibles, and co-insurance details.
- Any coverage limitations or exclusions.
This step prevents financial surprises for both the provider and the patient’s family.
2. Prior Authorization
ABA services usually require insurance authorization before therapy begins. Billing services handle all documentation, communicate with insurers, and secure approvals. This ensures claims will not be denied for lack of authorization.
3. Coding and Documentation
ABA therapy requires precise CPT coding. For example:
- 97151: Behavior identification assessment.
- 97153: Adaptive behavior treatment by protocol.
- 97155: Treatment with protocol modification.
- 97156: Family adaptive behavior treatment guidance.
Accurate coding ensures compliance and maximizes reimbursement.
4. Claims Submission and Management
Billing services use electronic systems to submit claims quickly and track their status. They follow up on unpaid claims and appeal denials to reduce revenue loss.
5. Compliance and Regulations
ABA billing providers ensure compliance with HIPAA guidelines, payer-specific requirements, and state regulations. This reduces the risk of audits, penalties, or claim rejections.
0 comments
Log in to leave a comment.
Be the first to comment.